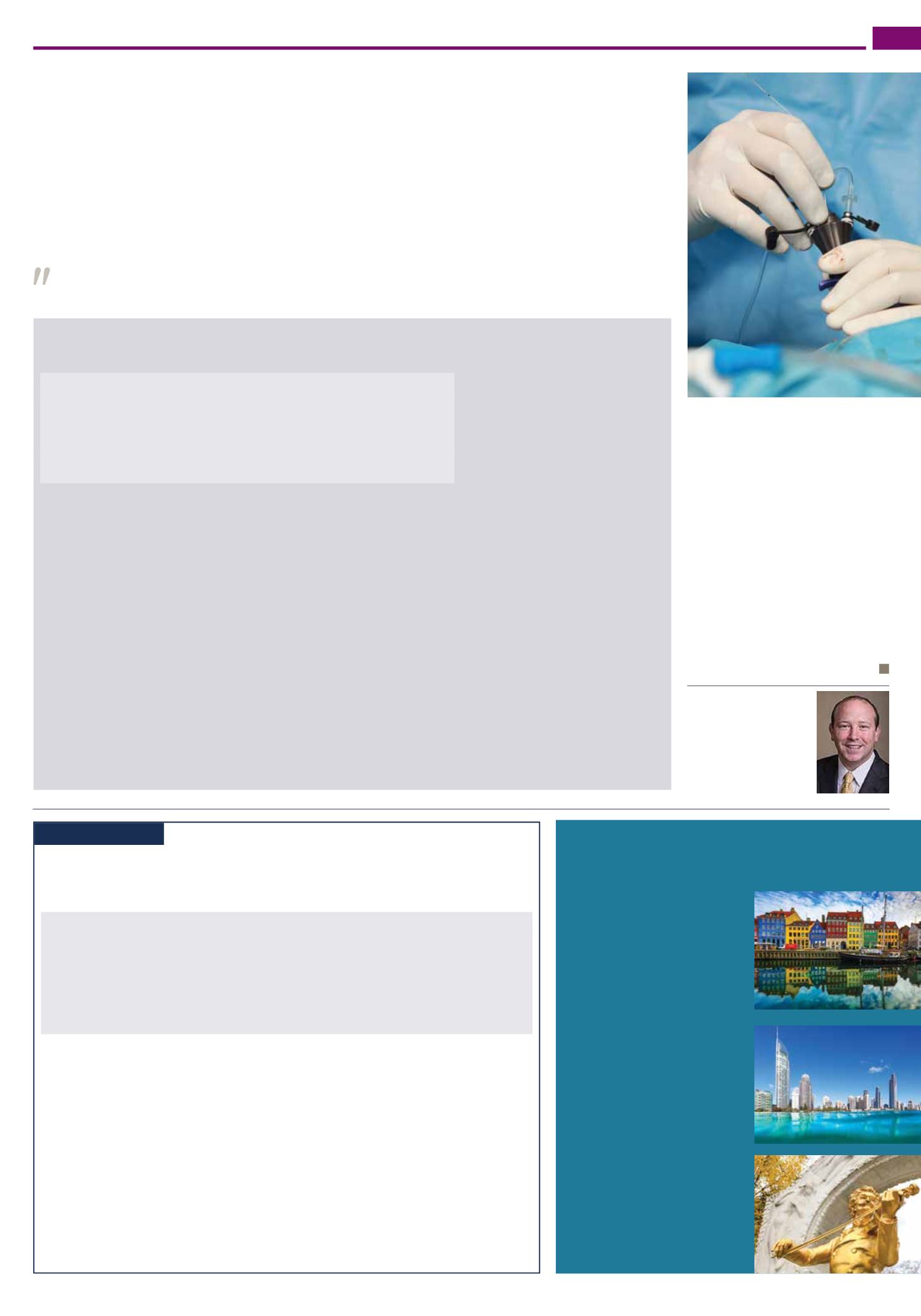
Robotic equals open surgery for prostate cancer
Comment by Thomas Guzzo, MD, MPH
T
his is the first published randomised trial
comparing outcomes between robotic
and open prostatectomy for men with
prostate cancer. The study included 308 men
undergoing surgery at a single centre. The au-
thors report no significant differences in short-
term urinary and sexual function outcomes at
6 and 12 weeks. There was also no significant
difference in positive margin rates between
surgical approaches.
The robotic patients did have significantly
less blood loss, a shorter length of stay, and
were less likely to have had an intraoperative
adverse event.
With the widespread adoption of robotic
surgery in the United States over the last dec-
ade, this trial is unlikely to have a significant
impact on practice patterns. This study does
potentially validate what we have already ob-
served clinically: regardless of approach, pros-
tatectomy functional and oncologic outcomes
are equivalent and more dependent on surgeon
expertise and experience than a machine. It
also demonstrates the potential short-term
benefits of robotic surgery including less blood
loss, less pain, and a shorter hospital stay.
However, I would caution readers when
interpreting these results that, in my opinion,
there is a significant methodologic flaw that
limits our ability to draw definitive conclusions
from this study. As noted in the methods sec-
tion, this study was performed by two surgeons
(one robot and one open) and therefore has
questionable generalisability to all urologists
who perform prostate cancer surgery. Addition-
ally, at the start of the trial, the robotic surgeon
had only completed 200 robotic prostatecto-
mies compared with the open surgeon who
had 15 years’ post-fellowship experience and
had already completed 1500 open prostatec-
tomies. With all due respect to both surgeons,
I am not sure that this was a fair comparison.
Dr Guzzo is Assistant
Professor of Urology
in Surgery, University
of Pennsylvania
Perelman Center for
Advanced Medicine.
Robot-assisted laparoscopic prostatectomy vs open radical retropubic prostatectomy
The Lancet
Take-home message
•
This randomised, multicentre phase 3 trial compared clinical outcomes of open vs robot-assisted
laparoscopic radical prostatectomy in 326 men with newly diagnosed early-stage prostate
cancer. Urinary function and sexual function were similar at 12 weeks post resection. Positive
surgical margin rates were also similar at 10% vs 15% in the open vs robot-assisted laparoscopic
prostatectomy groups, respectively (P = 0.21).
•
Robot-assisted laparoscopic radical prostatectomy is associated with clinical outcomes similar
to those achieved with open radical prostatectomy.
Abstract
BACKGROUND
The absence of trial data comparing
robot-assisted laparoscopic prostatectomy and
open radical retropubic prostatectomy is a crucial
knowledge gap in uro-oncology. We aimed to com-
pare these two approaches in terms of functional
and oncological outcomes and report the early
postoperative outcomes at 12 weeks.
METHOD
In this randomised controlled phase 3
study, men who had newly diagnosed clinically
localised prostate cancer and who had chosen
surgery as their treatment approach, were able to
read and speak English, had no previous history
of head injury, dementia, or psychiatric illness or
no other concurrent cancer, had an estimated life
expectancy of 10 years or more, and were aged
between 35 years and 70 years were eligible and
recruited from the Royal Brisbane and Women’s
Hospital (Brisbane, QLD). Participants were ran-
domly assigned (1:1) to receive either robot-assisted
laparoscopic prostatectomy or radical retropubic
prostatectomy. Randomisation was computer gen-
erated and occurred in blocks of ten. This was an
open trial; however, study investigators involved in
data analysis were masked to each patient’s condi-
tion. Further, a masked central pathologist reviewed
the biopsy and radical prostatectomy specimens.
Primary outcomes were urinary function (urinary
domain of EPIC) and sexual function (sexual domain
of EPIC and IIEF) at 6 weeks, 12 weeks, and 24
months and oncological outcome (positive surgi-
cal margin status and biochemical and imaging
evidence of progression at 24 months). The trial
was powered to assess health-related and domain-
specific quality of life outcomes over 24 months.
We report here the early outcomes at 6 weeks
and 12 weeks. The per-protocol populations were
included in the primary and safety analyses.
FINDINGS
Between Aug 23, 2010, and Nov 25,
2014, 326 men were enrolled, of whom 163 were
randomly assigned to radical retropubic prosta-
tectomy and 163 to robot-assisted laparoscopic
prostatectomy. 18 withdrew (12 assigned to radi-
cal retropubic prostatectomy and six assigned to
robot-assisted laparoscopic prostatectomy); thus,
151 in the radical retropubic prostatectomy group
proceeded to surgery and 157 in the robot-assisted
laparoscopic prostatectomy group. 121 assigned
to radical retropubic prostatectomy completed
the 12 week questionnaire versus 131 assigned to
robot-assisted laparoscopic prostatectomy. Urinary
function scores did not differ significantly between
the radical retropubic prostatectomy group and
robot-assisted laparoscopic prostatectomy group
at 6 weeks post-surgery (74.50 vs 71.10; P = 0.09) or
12 weeks post-surgery (83.80 vs 82.50; P = 0.48).
Sexual function scores did not differ significantly
between the radical retropubic prostatectomy
group and robot-assisted laparoscopic prostatecto-
my group at 6 weeks post-surgery (30.70 vs 32.70;
P = 0.45) or 12 weeks post-surgery (35.00 vs 38.90;
P = 0.18). Equivalence testing on the difference be-
tween the proportion of positive surgical margins
between the two groups (15 [10%] in the radical
retropubic prostatectomy group vs 23 [15%] in the
robot-assisted laparoscopic prostatectomy group)
showed that equality between the two techniques
could not be established based on a 90% CI with a
Δ of 10%. However, a superiority test showed that
the two proportions were not significantly different
(P = 0.21). 14 patients (9%) in the radical retropubic
prostatectomy group versus six (4%) in the robot-
assisted laparoscopic prostatectomy group had
postoperative complications (P = 0.052). 12 (8%)
men receiving radical retropubic prostatectomy
and three (2%) men receiving robot-assisted lapa-
roscopic prostatectomy experienced intraoperative
adverse events.
INTERPRETATION
These two techniques yield simi-
lar functional outcomes at 12 weeks. Longer term
follow-up is needed. In the interim, we encourage
patients to choose an experienced surgeon they
trust and with whom they have rapport, rather than
a specific surgical approach.
Robot-assisted laparoscopic prostatectomy
versus open radical retropubic prostatectomy:
early outcomes from a randomised controlled
phase 3 study.
Lancet
2016 Jul 26;[EPub Ahead
of Print], JW Yaxley, GD Coughlin, SK Chambers,
et al.
JOURNAL SCAN
Improved outcomes with early salvage radiotherapy inmen with detectable
PSA after prostatectomy for prostate cancer
Journal of Clinical Oncology
Take-home message
•
Salvage radiotherapy outcomes were examined in 1106 men with detectable PSA after radical prostatectomy for
prostate cancer. At a median follow-up of 8.9 years, tumour stage, Gleason score, and pre-salvage radiotherapy
PSA correlated with overall survival, cumulative incidence for biochemical recurrence (BcR), distant metastases,
and cause-specific mortality on multivariate analyses. The risks of BcR, distant metastases, and cause-specific and
all-cause mortality were significantly increased with each doubling of pre-radiotherapy PSA.
•
Reductions in BcR, metastases, and mortality may be achieved by using salvage radiotherapy at lower PSA levels.
The authors argue against prolonged monitoring of PSA levels that delays the start of salvage radiotherapy after
prostatectomy.
Abstract
PURPOSE
To describe outcomes of salvage radiotherapy (SRT)
for men with detectable prostate-specific antigen (PSA) after
radical prostatectomy for prostate cancer and identify as-
sociations with outcomes.
PATIENTS AND METHODS
A total of 1,106 patients received SRT
between January 1987 and July 2013, with median follow-up
8.9 years. Outcomes were estimated using Kaplan-Meier for
overall survival (OS) and cumulative incidence for biochemical
recurrence (BcR), distant metastases (DM), and cause-specific
mortality (CSM). Variable associations with outcomes used
Cox or Fine-Gray methods, as appropriate. Multiple variable
analyses used backward selection with P < 0.05 for retention.
RESULTS
In multiple variable analyses, pathologic tumour
stage, Gleason score, and pre-SRT PSA were associated
with BcR, DM, CSM, and OS; androgen suppression and
SRT doses > 68 Gy were associated with BcR; and age was
associated with OS. Each pre-SRT PSA doubling increased
significantly the relative risk of BcR (hazard ratio [HR], 1.30; P <
0.001), DM (HR, 1.32; P < 0.001), CSM (HR, 1.40; P < 0.001), and
all-cause mortality (HR, 1.12; P = 0.02). Using a pre-SRT PSA
cutoff ≤ 0.5 versus > 0.5 ng/mL, 5-year and 10-year cumulative
incidences for BcR were 42% versus 56% and 60% versus
68% (P < 0.001), DM 7% versus 14% and 13% versus 25% (P
< 0.001), CSM 1% versus 4% and 6% versus 13% (P < 0.001),
and OS of 94% versus 92% and 83% versus 73% (P > 0.05).
CONCLUSION
SRT outcomes are in part affected by factors
associated with prostatectomy findings but may be posi-
tively affected by using SRT at lower PSA levels, including
reductions in BcR, DM, CSM, and all-cause mortality. These
findings argue against prolonged monitoring of detectable
postprostatectomy PSA levels that delay initiation of SRT.
Improved metastasis-free and survival outcomes with
early salvage radiotherapy in men with detectable
prostate-specific antigen after prostatectomy for prostate
cancer.
J Clin Oncol
2016 Aug 01;[Epub ahead of print],
Stish BJ, Pisansky TM, Harmsen WS, et al.
There is a significant methodologic flaw that limits our ability to draw
definitive conclusions from this study.
Upcoming conferences 2016
OCTOBER
7–11 October | Copenhagen, Denmark
40th ESMO Congress
www.esmo.org/Conferences/ESMO-2016-Congress
10–12 October | Adelaide, Australia
Australian Gastroenterology Week
2016
www.agw2016.org.auNOVEMBER
15–17 November |
Gold Coast, Australia
43rd COSA Annual Meeting
cosa2016.org15–17 November |
Gold Coast, Australia
38th Annual Scientific Meeting of the
ANZ Breast Cancer Trials Group
cosa2016.orgDECEMBER
4–7 December | Vienna, Austria
17th World Conference on Lung
Cancer
wclc2016.iaslc.orgPROSTATE
VOL. 1 • No. 3 • 2016
5








